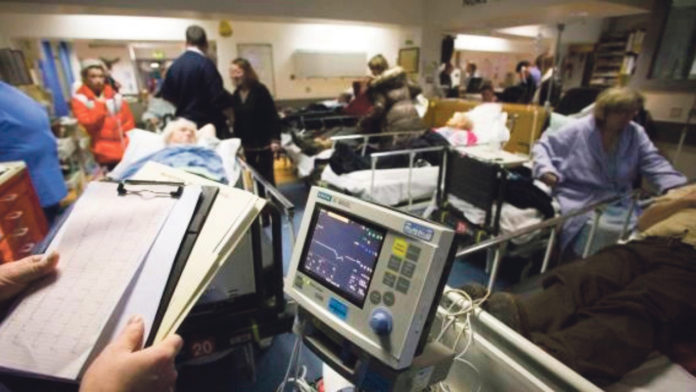
IT’S midnight at University Hospital Limerick and there are trolleys stacked one and two deep along the corridors in the emergency department.
This is not a bank holiday weekend nor a Saturday night drunk tank. It’s Tuesday, November 20 and they have run out of trolleys.
Earlier this evening, the very waiting room of the emergency department was so crowded that people were sitting on the floor for lack of chairs.
As a journalist, I have been writing about this situation, listening to staff, patients and families describe it for years.
Now, I’m seeing this horror as a patient on one of those trolleys.
I’ve been told I need a bed in hospital and I expect a long wait. I’m seen within half an hour of arriving and examined within a couple of hours. I’m told they will find a trolley and I have an IV inserted.
Then it all stops.
There are no trolleys. Outside the treatment area of the emergency department, where patients wait to be called for examination and treatment, they have run out of chairs. People are sitting on the floor or in wheelchairs. These are almost all patients and the few who have brought support are accompanied by just one person, not a contingent of family or mates.
The wait is so long that a doctor comes out to ask if he can inject me with intravenous antibiotics there in the waiting area.
It’s far from ideal but these are dedicated people whose first concern is treating patients as best they can.
Later in the evening, I’m brought to a corridor where patients are lined up end to end. It’s nothing short of dystopian.
The lady behind me – a pensioner who arrived as an emergency with no nightwear, change of clothes or any kind of comforts – was on a trolley for more than 30 hours since Monday morning.
The woman in front of me, who looks even older, has also been waiting since Monday. Of six of us in this corridor, I can see that three of us could have been treated in a bed in Ennis, St John’s or Nenagh Hospitals. That’s where they are hoping to send us.
We don’t need to be here.
But the only other way into a hospital bed is through the Medical Assessment Units and their appointments are all booked days ahead. Respiratory disease like pneumonia won’t hang around.
My GP is one of the many who send their patients here as their only hope of getting them a bed.
A look around the immediate vicinity reveals trolleys staggered two on two in the area around the nurses station, where the most critical patients are being kept.
In every direction, there are occupied trolleys and I’m told there are more in places that I can’t see.
The isolation bays have also been pressed into use.
Some patients are resigned to the long wait. Some are in desperate discomfort. The trolleys are unimaginably uncomfortable, narrow and padded with just a couple of inches of foam. Elderly people, with bones frail as sparrow skeletons are tossing and turning to find some comfort.
They’ve run out of blankets, which is not a problem in my particular neck of the woods because the body heat is turning the corridor into a sauna.
Every member of staff in this department is unfailingly courteous, professional and kind.
But it is clear they are stretched to breaking point.
The nurse taking blood pressure has to slide her equipment between the wall and the trolleys. There’s barely room for her to use it.
Two people pushing equipment or a wheelchair cannot pass in this space. If they meet one has to back up.
I remark to the nurse about the sheer density of people, some of them who can walk and some who could not move if there was an emergency.
“What happens if there’s a fire?” I ask. Her face is grim when she answers. “There hasn’t been a fire”. The word that hangs unsaid is “yet”.
It can’t be stressed enough that we are all people diagnosed as being ill enough to need a proper bed in a hospital ward. That we are receiving any treatment at all is a testament to the dedication of the staff.
But treatment requires that doctors ask patients questions. Personal ones, in an environment where there is no privacy whatever.
We try not to listen but after the first doctor’s round, one woman has had to talk about her severe psychiatric condition and her need for medication.
We know that another young woman is taking the contraceptive pill. A man further along is being treated for alcoholic liver disease.
If anyone here has a sexually transmitted disease, you could put money on them taking the risk of not revealing it and suffering the possible consequences.
There’s no choice for medical staff but to discuss these matters here. Diagnosis and the administration of drugs must be based on medication already prescribed.
Most of us hope we will never see any of our fellow patients again. We are all now in possession of information we didn’t want to hear or reveal.
A young man who has been with us in the corridor for several hours is taken away to a private bay. When I meet him later on the way to the toilet, he is wearing a cardboard mask across his mouth.
He tells me they suspect he may have TB. I can’t be sure if that is correct but it’s evident they are now taking precautions against something they fear is infectious.
It’s 4am and sleep is only possible in snatches. The lights are on full blast, the noise from the porters and security guard station around the corner is beyond loud and people are passing through constantly. Because it is, after all, a corridor.
Medical staff have to shout out patients’ names to find the person they have been sent to administer to. A vague description of location – in our case, ‘resuc (resuscitation) corridor’ is all the have to go on.
Throughout the night, porters arrive enquiring if there are free trolleys. At one stage, another patient on a trolley has to be put in this area.
An exasperated nurse asks “where, for God’s sake?”
There is not an inch of room for the new arrival. Already, I could comb the hair of the woman on the next trolley with my toes, we are pushed so close together.
We are asked if we would like something to help us sleep and most say yes, but nothing comes of it.
When I see my own notes afterwards, they say “patient slept comfortably”.
There are three toilets in the immediate area. One is out of order, another has a trolley across the door and at 2am, the third one is filthy, with bits of toilet tissue, stains and splashes covering the floor area. The toilet seat itself is destroyed with urine. There’s one cleaner on duty and I point out the problem but two hours later it’s still in the same disgusting state.
There are other facilities outside the doors of the emergency department. For those who can walk to them.
There’s nowhere to wash the sweat off or to change clothes. A woman trying to put on pyjamas in the corridor abandons all hope of modesty and does her best to change when no-one is looking.
Sandwiches, soup and tea arrive during the evening on a push-cart. By the time they reach the third trolley, they’ve run out of soup.
A sandwich is the only food anyone can expect until morning, provided they don’t run out of those.
Around 8am, a team of doctors led by a consultant arrive to speak to the elderly lady in front of me. The consultant turns to his team to order that she is prioritised for a bed.
Her daughters come to visit a little later but there is nowhere for them to sit so they stand beside her, moving aside every time someone else needs to get past. A private conversation is impossible but she tells them they have promised to get her on to a ward.
“Hardly worth my while, now,” she says stoically.
By 4pm on Wednesday, 28 hours after I arrive at the emergency department, an ambulance crew member calls my name and announces he’s taking me and another patient to Ennis. The prioritised elderly lady is still on her trolley.
I’m no hero, but I tell a nurse I don’t want a bed ahead of this unfortunate woman. I’m told her needs have to be catered for here, at the acute hospital. Eventually.
The journey to Ennis hospital feels like a prison break and as I close the door on my spacious, spotless, one-patient public room, I feel as if I have made a lucky escape.


