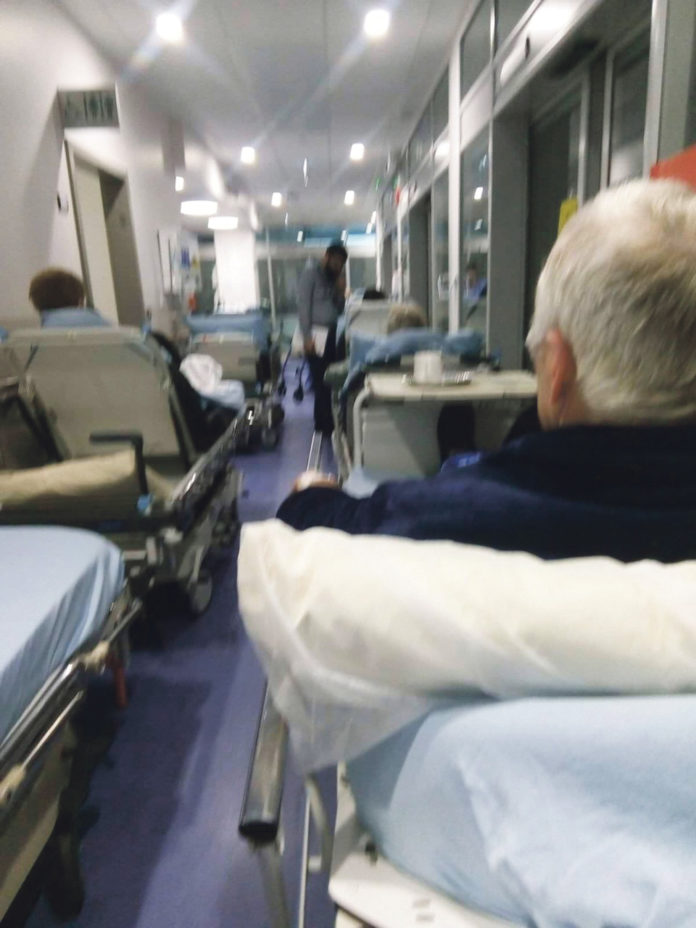
MORE than 5,000 patients who went to the Emergency Department in University Hospital Limerick left without being discharged or finishing treatment last year.
That’s according to the latest compiled figures released under Freedom of Information to the Irish Examiner, and does not allow for months for which data is not available due to a cyberattack on the HSE system.
University Hospital Limerick was fourth highest in the country of hospitals most impacted by what are known as “did not waits”, with 5,334 patients walking away.
Ahead of Limerick were the Mater Hospital and Tallaght Hospital in Dublin and Our Lady of Lourdes in Drogheda.

- External Walls: Up to €8,000 Grant
- Attic: Up to €1,500 Grant
- Cavity Walls: Up to €1,700 Grant
- Internal Dry Lining: Up to €4,500 Grant
The patients who left were not officially discharged and did not complete treatments that may have been started while in the emergency department.
A spokesperson for University Hospital Limerick said the figure “illustrates the picture in emergency departments nationwide.”
The HSE’s national press office said: “The purpose of emergency departments is to deal with serious and unexpected illness and injury. Many people, whose clinical needs could be more appropriately addressed by self-care, pharmacists, GPs, GP Out of Hours Services and Minor Injury Units, continue to attend Emergency Departments.
“In this context, it is inevitable that emergency departments and their associated hospitals, whose capacity is exceeded by such demand, must clinically prioritise those who must be treated first and those who may need to wait, or attend a more appropriate care setting.
“To ensure this process is clinically safe for patients, Irish hospitals use the internationally tested Manchester Triage Tool, which prioritises patients into a number of categories based on their clinical needs. Where a patient is seriously ill or injured, their needs will be prioritised above those with less serious conditions.
“Ideally, hospitals would be in a position to treat patients on their arrival. However, as demand inevitably overtakes capacity, prioritisation and consequential waiting may occur. In this regard, some patients with less serious needs may choose to avail of alternative options.”

