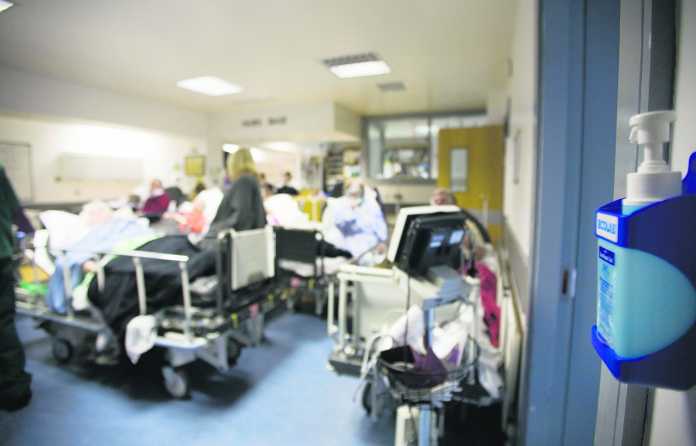
UNION representatives of staff at University Hospital Limerick (UHL) have once again raised the issue of overcrowding with management as the hospital hit 50 consecutive days as the most overcrowded in the country.
While the Irish Nurses and Midwives Organisation (INMO), who keep the daily national Trolley Watch count, agree with hospital management that attendances and trolley numbers have been very high across this summer, the union say they are still seeking solutions.
INMO Assistant Director of Industrial Relations, Mary Fogarty, told the Limerick Post that “the level of persistent overcrowding is a serious concern for nurses at UHL”.
“The INMO has raised the concerns of our members again this week with senior management, who were not in a position to provide any plan as to how the hospital will manage the winter months,” Ms Fogarty said.
“The volume of patients on trolleys at UHL this summer is excessively high in comparison to other acute hospitals nationwide. All in-patient wards are overcrowded, along with the Emergency Department, leading to poor outcomes for patients and work related stress for nurses who have to constantly work in an overcrowded workplace.”
The Limerick Post has kept an ongoing record of where the Dooradoyle hospital stands in terms of overcrowding within the national rankings, according to the Trolley Watch figures operated on weekdays by INMO.
On Thursday of this week (July 27), the hospital became the most overcrowded in the country for 50 consecutive days, with 99 admitted patients waiting on trolleys or in overflow areas for a regular hospital bed on day 50.
In response to the issue, first reported by the Limerick Post, a spokesman for University Hospital Limerick (UHL) told this newspaper that “over the past 50 days, and for some significant length of time prior to that, we have been dealing with a significant increase in numbers of patients – many of them elderly and frail people and other high-acuity patients with specific care requirements – presenting to the Emergency Department (ED)”.
“From June 7 to July 27, a total of 11,204 patients have attended the ED, an average of 224 patients every 24 hours,” the spokesman said.
“This is far in excess of the 195 daily average attendance figure recorded during 2019, the last full year prior to the Covid-19 pandemic.
“At times it has far exceeded even the average figure for the month, with particular high experienced on June 9-10 (264), June 19-20 (259), and June 26-27, which had the highest daily attendance figure of the month, with 292 patients attending.
“UL Hospitals Group’s shortfall in bed capacity, particularly in UHL, has been repeatedly acknowledged, and, as highlighted in the Deloitte Report, remains the fundamental driver of hospital overcrowding in the Mid West. This problem will continue until there is a substantial increase in bed capacity.”
The UL Hospitals Group (ULHG) is made up of six hospitals across the Mid West: University Hospital Limerick, University Maternity Hospital Limerick, Ennis Hospital, Nenagh Hospital, Croom Orthopaedic Hospital, and St John’s Hospital Limerick.
The ULHG spokesman said that the shortage of hospital beds means hospitals in the Group have an ongoing balancing act to perform with the “needs of its inpatients patients; of the sickest patients most in need of immediate attention on our emergency and urgent care pathways; and of those who are waiting for surgery.”
“All too often this means that admitted patients experience significant waits for hospital beds, and this is not the standard of care we wish to provide for our patients. We apologise to anyone who has been so impacted.”
“Our staff at all levels across UL Hospitals Group are working hard to reduce these wait times.”
Work is progressing on a new 96-bed block for the hospital and planning is moving forward for building a second 96-bed block on the Dooradoyle hospital campus.
“We continue to follow our escalation plan to reduce pressure on the ED and improve patient flow across our sites. Measures that have been taken include the opening of surge capacity across all sites; transfers of patients on trolleys to our inpatient wards; reductions in scheduled care; additional ward rounds by medical teams to expedite discharges or to identify patients suitable for transfer to Ennis, Nenagh, and St John’s Hospitals; and working closely with our colleagues in HSE Mid West Community Healthcare in order to expedite discharges,” the spokesman concluded.


